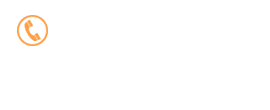دکتر مجید حقیقت
متولد شهریور ماه 1345 در خانواده متوسط اصفهانی , دوران تحصیلات ابتدائی تا دیپلم را در مدارس اصفهان گذرانده و درسال 1364 در رشته پزشکی دانشگاه اهواز آغاز به تجصیل نمود.
در امتحان جامع پره انترنی اسفند 1369 بطور مشترک رتبه اول را کسب کرده و در سال 1371 بعنوان پرشک عمومی فارغ التحصیل شد . درسال 1373 با کسب رتبه اول داوطلبان دستیاری رشته تخصصی ارولوژی ( جراحی کلیه و مجاری ادراری ) دانشگاه اصفهان , ادامه تحصیل داده و در سال 1377 با کسب بورد تخصصی ارولوژی و رتبه اول دانشگاه فارغ التحصیل شد.
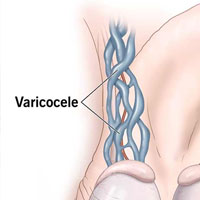
برای اولین بار در شهر اصفهان استفاده از میکروسکوپ را در جراحی های ناباروری (میکرو سرجری) آغاز کرد و هم اکنون با عضویت EAU انجمن ارولوژی اروپا ( www.uroweb.org ) مشغول ارائه خدمات درمانی به هموطنان میباشد.